Surgery for Herniated Disc
Herniated Disc Surgery in Milwaukee, WI
A herniated disc can be a painful and debilitating condition, affecting daily activities and overall quality of life. If left untreated, it can lead to chronic pain and more severe spinal complications.
Fortunately, advancements in minimally invasive spine surgery have made treatment more effective and accessible.
What is a Herniated Disc?
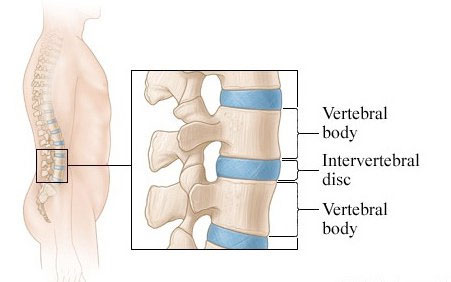
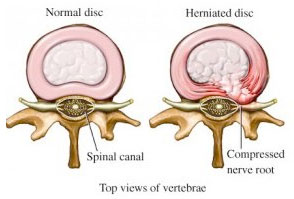
A herniated disc – sometimes called a slipped or ruptured disc – occurs when the soft inner gel of a spinal disc pushes through its tougher outer layer. This can result in nerve compression, leading to pain, weakness, or tingling sensations. Herniated discs commonly occur in the lumbar (lower back) and cervical (neck) spine, where movement and pressure on the spine are most frequent.
An experienced back surgeon can diagnose and treat a herniated disc using various approaches. These may include slipped disc surgery as well as non-surgical treatments like physical therapy, medication, and epidural injections.
When conservative treatments fail to provide relief, minimally invasive surgical procedures offer an effective alternative to treat slipped discs and other spine conditions. These procedures use smaller incisions, reduce trauma to surrounding tissues, and promote faster recovery times compared to traditional open surgery to repair a herniated disc.
How Is a Herniated Disc Diagnosed?
Diagnosing a herniated disc begins with a detailed clinical evaluation. A spine specialist reviews your symptoms, including radiating pain, numbness, weakness, or tingling. The doctor will ask when the pain started, how it has progressed, and what activities make it worse or better.
A physical and neurological exam follows. This may include reflex testing, muscle strength checks, sensory testing, and range of motion evaluation. These steps help determine if a nerve is being compressed and how severely it is affected.
Imaging studies often confirm the diagnosis. An MRI is considered the gold standard for identifying disc herniation and nerve compression because it clearly shows soft tissues. A CT scan may be used when MRI is not appropriate. X-rays do not show soft tissue discs but can help rule out fractures, instability, or degenerative changes.
Diagnostic findings guide treatment decisions. Imaging must match the patient’s symptoms before surgery is considered. Many people have disc bulges on imaging without pain. Accurate interpretation prevents unnecessary procedures.
If you are experiencing persistent symptoms such as sciatica nerve pain, early evaluation by a spine specialist is important. Dr. PRPA carefully reviews each case and determines whether non-surgical care or surgery is the best next step. Patients across our locations receive thorough evaluations before any surgical recommendation is made. Learn more from our previous surgical cases.
Am I a Candidate for Herniated Disc Surgery?
Several factors contribute to the likelihood of developing a herniated disc. Certain lifestyle habits, medical conditions, and genetic predispositions increase the risk of spinal disc deterioration. Those most at risk include:
- Adults between 30 and 50 years old, as spinal discs naturally weaken with age
- Individuals with physically demanding jobs that involve heavy lifting or repetitive bending
- Those who are overweight, putting added stress on the spine
- People with a family history of spinal disorders
- Smokers, as reduced oxygen flow to spinal tissues can weaken discs over time
Common Symptoms of a Herniated Disc:
A herniated disc can cause a range of symptoms, depending on the location and severity of the condition. Some individuals may experience mild discomfort, while others face debilitating pain that interferes with daily life. Recognizing the signs early can help prevent further complications and allow for more effective treatment.
- Radiating pain in the back, buttocks, legs, or arms
- Numbness or tingling in the affected area
- Muscle weakness or difficulty moving
- Increased pain when sitting, bending, or lifting
- Trouble walking or maintaining balance
If these symptoms persist, seeking an evaluation from a spine specialist is essential.
What Does Treatment Look Like?
A herniated disc operation is not always necessary. Many patients experience relief through non-surgical methods, while others require surgical intervention based on the severity of their condition.
Non-Surgical Treatment Approaches
- Physical Therapy – Exercises that strengthen core muscles and improve spinal flexibility
- Pain Management – Anti-inflammatory medications, muscle relaxants, and targeted pain relievers
- Epidural Injections – Corticosteroid injections to reduce inflammation around the affected nerve
Minimally Invasive Herniated Disc Surgery
If conservative treatments fail to provide relief, minimally invasive techniques such as microdiscectomy or endoscopic discectomy may be recommended. These procedures involve small incisions and specialized instruments to remove the damaged portion of the disc, reducing nerve pressure while preserving surrounding tissues.
At Branko Prpa M.D. Spine Surgery, each patient receives a customized treatment plan tailored to their specific condition.
Recovery & Rehabilitation
Recovery from herniated disc surgery in Milwaukee varies depending on the procedure and the individual’s overall health. However, most patients experience significant pain relief and improved mobility within a few weeks.
General Recovery Timeline:
- First Few Days – Mild discomfort is common, but patients can walk and perform light activities
- Week 2-4 – Working with a physical therapist to improve strength, posture, and flexibility
- Week 6-12 – Most patients resume work and normal activities with some restrictions
A well-structured rehabilitation program plays an essential role in recovering from ruptured disc surgery and in preventing future spinal issues down the road.
Types of Herniated Disc Surgery We Perform
Microdiscectomy
Microdiscectomy is one of the most common procedures for treating a symptomatic disc herniation. During this procedure, the surgeon removes the portion of the disc pressing on the nerve through a small incision. Specialized instruments and magnification allow precise removal while preserving surrounding tissue.
Endoscopic Discectomy
Endoscopic discectomy uses a small camera and instruments inserted through a tiny incision. This technique allows the surgeon to view and remove the herniated disc fragment with minimal disruption to muscle and tissue. It often results in less post-operative discomfort and a quicker return to daily activities. Patients receive detailed guidance on how to prepare for back surgery before the procedure.
Lumbar spine (lower back)
Sciatica frequently results from a herniated disc in the lower back. Pressure on one or several nerves that contribute to the sciatic nerve can cause pain, burning, tingling, and numbness that radiates from the buttock into the leg and sometimes into the foot. Usually one side (left or right) is affected. This pain often is described as sharp and electric shock-like. It may be more severe with standing, walking or sitting. Along with leg pain, you may experience low back pain.
Cervical spine (neck)
Symptoms may include dull or sharp pain in the neck or between the shoulder blades, pain that radiates down the arm to the hand or fingers, or numbness or tingling in the shoulder or arm. The neck pain may increase with certain positions or movements of the neck.
Why Trust Branko Prpa M.D.?
Choosing the right spine specialist is vital for achieving the best outcome. Dr. Branko Prpa is a trusted leader in minimally invasive spine surgery in Milwaukee, offering personalized, patient-centered care that prioritizes comfort, precision, and long-term results.
Patients benefit from:
- Same-dayevaluations for urgent cases
- Advanced minimally invasive techniques that promote faster recovery
- A commitment to comprehensive care, from diagnosis through rehabilitation
Residents of Milwaukee looking for expert herniated disc treatment can rely on Branko Prpa M.D. Spine Surgery for compassionate care and cutting-edge solutions. Schedule a consultation today to take the first step toward relief and recovery.
FAQ’s
How do I know if my back pain is from a herniated disc?
Back pain from a herniated disc often feels different from simple muscle strain. You may notice pain that travels into your arms or legs, along with numbness, tingling, or weakness. If your symptoms are not improving or are getting worse, a spine specialist can perform a physical exam and order imaging – such as an MRI – to determine the exact cause.
Can a herniated disc heal without surgery?
Yes. Many people recover without surgery. Physical therapy, medication, activity changes, and epidural injections often reduce inflammation and relieve pressure on the nerve. Surgery is usually considered only if pain continues or symptoms progress despite these treatments.
When is herniated disc surgery necessary?
Surgery may be recommended if pain is severe, nerve compression is causing weakness, or daily activities become difficult due to ongoing symptoms. The decision is based on how much the condition is affecting your quality of life and whether non-surgical care has provided relief.
How long does it take to recover from herniated disc surgery?
Recovery depends on the procedure and your overall health. Many patients notice meaningful pain relief within a few weeks. With guided rehabilitation, most people return to normal activities within 6 to 12 weeks.
Is minimally invasive herniated disc surgery safe?
Minimally invasive spine surgery is widely used and has a strong safety record when performed by an experienced surgeon. Smaller incisions mean less disruption to surrounding tissue, which often leads to reduced discomfort and a smoother recovery.
